How to Stop Lichen Sclerosus Itching: Red and Blue Light Therapy at Home
As a midwife and PBM specialist, I’m seeing more and more women with Lichen Sclerosus (LS) where the main misery is constant itching, not advanced whitening and scarring. If that’s you, blue light plus gentle red/NIR can be a smart, research‑aligned, non‑burning option - and yes, you can do this at home with the Fringe Pelvic Wand stacked with the Solasta laser.
If you are living with Lichen Sclerosus (LS), you know that the "misery factor" isn't always about visible scarring, it’s that relentless, sanity destroying itch.
There is good news - and tools that you can use at home. Modern light therapy - specifically Blue and Red light offers a non-burning, research-backed way to calm the itch and support skin barrier repair right from your bedroom.
Key Takeaways: LS and Light Therapy
The Cause: Relentless itching is often caused by overactive mast cells (immune cells) and hypersensitive nerves.
The Tech:Blue light (415 nm) targets surface itching, while Red/NIR light (630–830 nm) supports deeper tissue healing.
The Research: A 2024 study showed a 50% reduction in itch using blue diode light, with results lasting up to 16 weeks.
The Strategy: Use the Fringe Wand for daily symptom relief and the Solasta Laser for deeper structural changes like scarring or thinning.
Circadian Rhythm: Avoid using blue light on the vulva at night to ensure your skin stays in repair mode while you sleep.
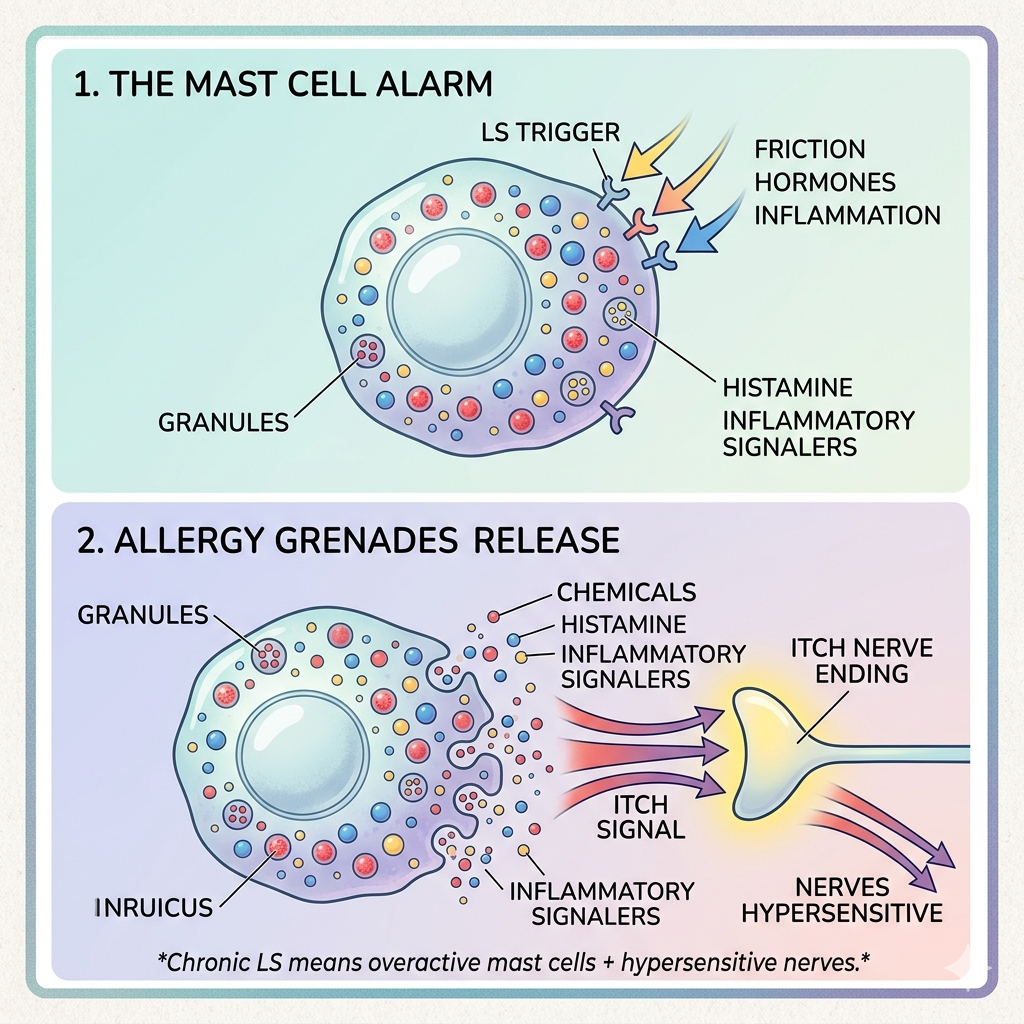
Why Does LS Itch So Much? Meet Your "Mast Cells"
LS is a chronic inflammatory condition. That crawling or burning sensation is usually caused by mast cells.
Think of mast cells as tiny "security grenades" living just under your skin. When LS triggers them, they degranulate (disintegrate), releasing histamine and other chemicals that talk directly to your nerve endings. Over time, these nerves become hypersensitive, leading to a chronic cycle of itching and burning even when the skin doesn't look "atrophic" yet.
Lichen Sclerosus = overactive mast cells.
How Photobiomodulation (PBM) Targets the Itch
We use specific wavelengths of light to "talk" to these cells and tell them to calm down. Unlike surgical lasers, PBM uses low-level light that does not burn or cut tissue.
Blue Light (415 nm): This is the heavy hitter for itching. It penetrates the very top layer of the skin to soothe overactive nerves and stop mast cells from dumping "itch chemicals."
Red & Near-Infrared Light (630–830 nm): These wavelengths go deeper. They improve microcirculation and reduce "raw" feelings, helping the skin repair its protective barrier.
A 2024 clinical study using a blue diode laser for vulvar LS (12 women) showed a 50% or greater reduction in itch and pain scores for most participants, plus visible improvements in redness and fissures, with effects still present at 16‑week follow‑up. The wavelength and power density used in that study are in the same neighborhood as what the Fringe wand delivers to superficial vulvar tissues, which is why I’m comfortable saying we’re not just guessing - we’re matching our approach to the emerging data.
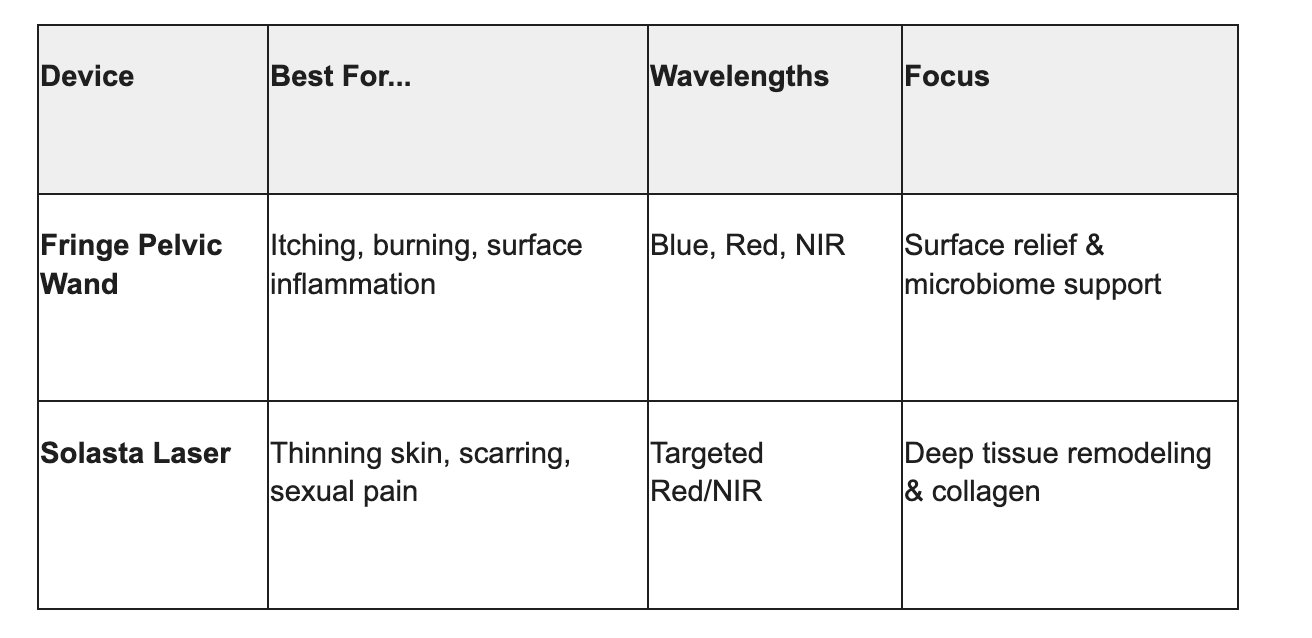
The Power Couple: The Fringe Wand & Solasta Laser
I recommend a "stacking" approach to cover both symptom relief and long-term tissue health:
Pro Tip: If itch is your main problem, the Fringe Wand is an excellent first step. If you already have significant scarring, adding the Solasta Laser provides the higher therapeutic dose needed for structural change.
The No-Go on Tanning Beds
Some women find temporary relief in tanning beds. While the UV light does reduce itch, the risk is too high. LS already carries a higher risk of vulvar cancer, and unregulated UV exposure significantly raises that danger. PBM gives you the benefits of light without the DNA-damaging UV rays.
Timing Matters: Don't Use Blue Light at Night
Your skin has its own internal "clock." Blue light signals to your cells that it is daytime. If you use the Blue Light mode on your vulva right before bed, you may disrupt the "repair mode" your skin enters during sleep.
Daytime: Use Blue Light (Fringe Wand) in the morning or afternoon.
Nighttime: If you need relief before bed, use Red/NIR mode only.
Frequently Asked Questions (FAQ)
Is photobiomodulation (PBM) safe for the vulva? Yes. PBM uses "cold" LED or laser light that does not produce heat or damage cells. It is a gentle, evidence-based way to manage inflammation without downtime.
How long does it take to see results? Most women notice a decrease in itching within 1 - 2 weeks. For deeper changes like improved skin elasticity or reduced scarring, consistent use for 8–12 weeks is typically required.
Can I use the Fringe Wand while using steroid creams? Yes. Light therapy can improve skin health, making your standard medical treatments more effective. Ensure your skin is clean before your light session for best penetration, then apply your cream afterward.
Does blue or red light therapy hurt? Not at all. You may feel a very slight, warmth, but there is no pain, peeling, or irritation.
Where can I buy your recommendedslight warmth, devices? You can find the Fringe Pelvic Wand and Solasta Laser directly in my online shop, with protocols designed to align with the latest LS research.
Additional Resources:
https://blog.tracydonegan.org/blog/compare-red-light-therapy-vaginal-wands
https://blog.tracydonegan.org/blog/red-light-therapy-and-vulvar-lichen-sclerosus