Painful Intercourse & Burning? How Red Light Therapy Soothes Provoked Vestibulodynia
What Is Provoked Vestibulodynia?
Provoked vestibulodynia (PVD) is pain at the entrance of the vagina that appears when the area is touched – with a tampon, penis, finger, speculum, or even tight clothing.
Women often describe the pain as burning, stinging, or cutting, and it can linger long after the contact is over. Millions of women worldwide live with vulvar pain like PVD, up to 1 in 4 may experience some form of it over a lifetime.
It often starts subtly, often manifesting as general ‘soreness after sex’, a string of yeast infections, or irritation that never fully clears – and over time the nerves in the entrance to the vagina become so sensitive that even gentle touch feels like burning.
Clinically, the vestibule often looks “normal,” which is why so many women are told that everything is fine while they are living with significant pain. (The vestibule sits between the inner lips (labia minora) and surrounds two openings: the pee hole (urethra) and the vaginal opening).
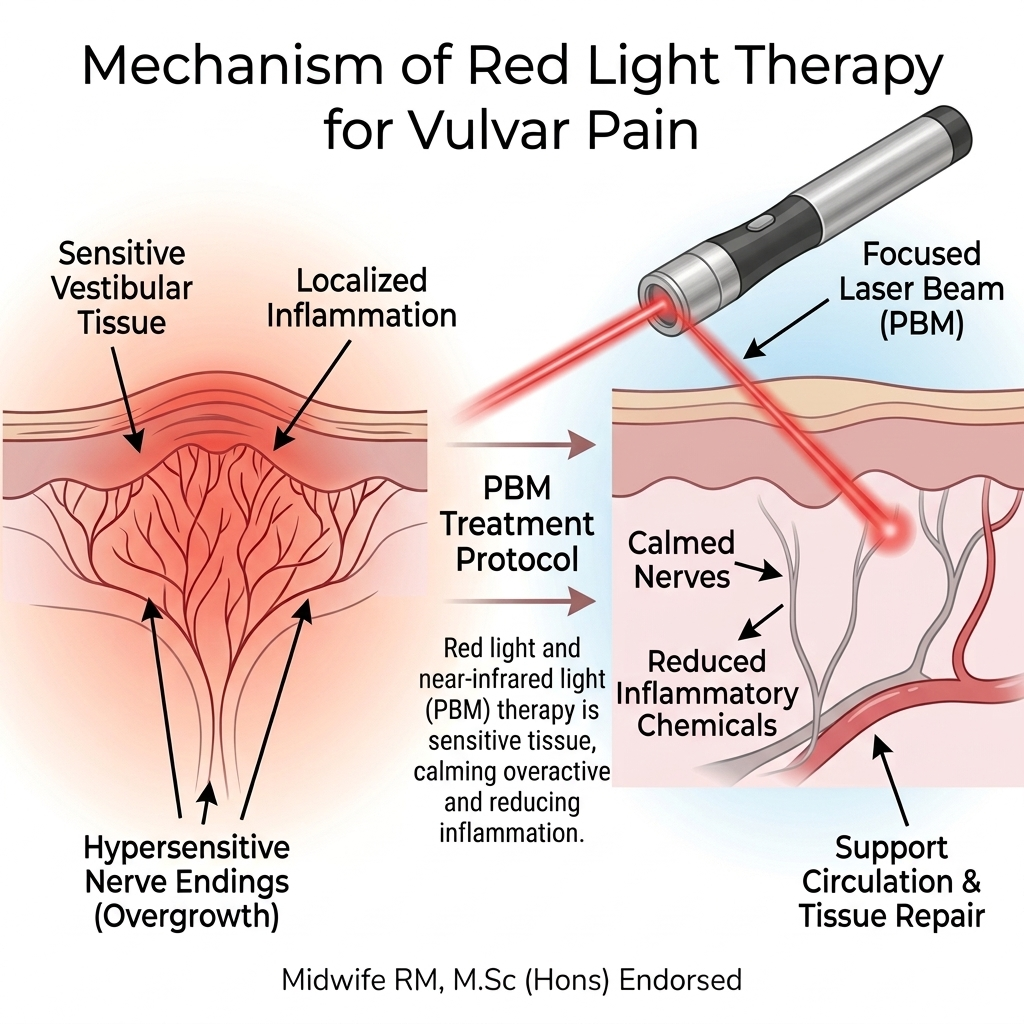
Under the surface, research shows three recurring themes:
· Local inflammation in the vestibular tissue.
· Overgrowth and sensitization of pain‑carrying nerve endings.
· Pelvic floor muscles that are tight and guarding around the opening.
In other words: this is a real, body‑based condition that deserves targeted treatment, not reassurance and dismissal (or the suggestion to have a glass of wine and relax….)
How Red Light Therapy Can Be Used
Photobiomodulation (PBM), also called low‑level laser therapy or “cold laser,” uses low‑intensity red and near‑infrared light to influence cell behavior without heating or damaging tissue.
At the level of the vestibule, photobiomodulation can:
· Reduce inflammatory chemicals in the tissue
· Calm overactive pain nerves
· Support local circulation and tissue repair
· Create a local analgesic effect that makes touch more tolerable
Because the vestibule is very superficial and highly innervated, it is an ideal target for this kind of light.
Free standard shipping + tailored protocol based on your health history and symptoms.
Let’s Look at the Emerging Evidence
Let’s anchor this in actual research data, not hype.
Study 1: Low‑Level Laser Directly to the Vestibule
A double‑blind, randomized, placebo‑controlled pilot trial used an 820 nm low‑level laser for women with PVD.
· 34 women were randomized to active laser or sham.
· Treatment: 12 sessions, twice a week for 6 weeks, targeting multiple points around the vestibule.
· Results:
o 78% of women in the laser group reported clinical improvement in pain versus 44% in the placebo group.
o About 57% of those who improved maintained benefit at one year.
o No side‑effects were reported.
Translation: a structured series of laser sessions produced meaningful, durable pain reduction for many women.
Study 2: Red + NIR PBM for Vulvar Pain in PVD
A newer randomized controlled trial used a PBM array with red and near‑infrared light in women with PVD.
· 15 sessions over roughly 8 weeks, delivered in five stages with gradually increasing exposure.
· Light was applied to the vestibule, perineum, and sacral region.
· Women receiving real PBM had significantly greater reductions in:
o Pain with tampon insertion
o Pressure‑pain sensitivity at the vestibule
o Vulvar pain questionnaire scores
· Many reached at least a 30% reduction in local pain sensitivity – the usual threshold for “clinically meaningful” improvement.
Again, treatment was well tolerated, and no serious adverse events were reported.
How a Handheld Laser Like Solasta May Help You
When used on the vulvar vestibule under professional guidance (my tailored protocol and check ins), a handheld home laser device aims to:
· Reduce local inflammation in the vestibular tissue.
· Down‑regulate hypersensitive nerve endings that fire with light touch.
· Support tissue repair and microcirculation.
· Reduce pain enough to make pelvic floor work, dilator therapy, and step‑by‑step return to intimacy more achievable.
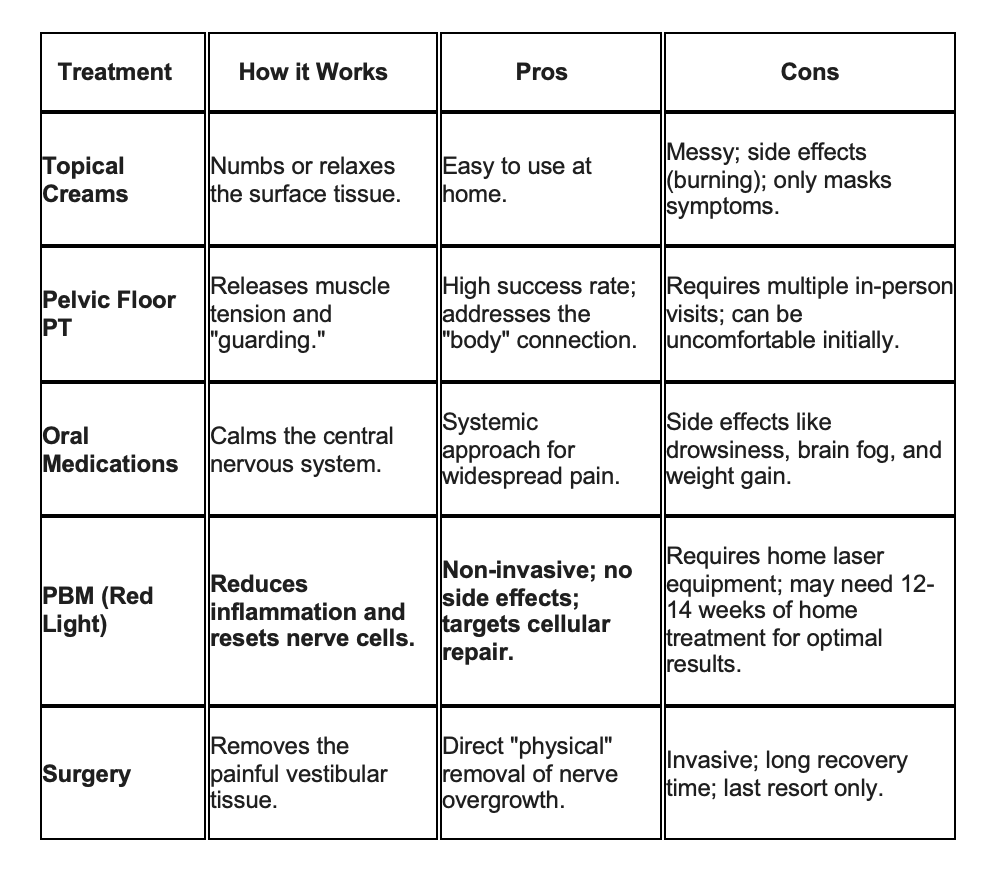
What Treatment Typically Looks Like
Protocols are always individualized, but the research points to a clear framework you can do at home:
· Frequency: 2 - 3 sessions per week
· Duration: Around 6–8 weeks (12–15 sessions in total)
Most women feel little during treatment – sometimes a gentle warmth, often nothing at all. There should be no burning or intense heat.
Why This Is Not a Solo Fix – And Still Worth Considering
PVD is multifactorial. Laser alone is not a cure‑all, and the data support PBM as part of a multimodal strategy, not a stand‑alone miracle.
That strategy often includes:
· Pelvic floor physiotherapy
· Attention to hormonal status and irritants
· Lubrication and graded exposure to touch
· Support for the emotional and relational impact of pain
-
While every woman’s "pain map" is different, clinical protocols typically suggest 2 to 3 sessions per week for a minimum of 6-8 weeks. Most women begin to notice a decrease in "sharpness" or burning after the first 4 sessions as the cellular inflammation begins to subside.
-
Yes. Unlike traditional ablative lasers used in surgery, Photobiomodulation (PBM) is a "cold laser." It does not cut or burn the tissue. It uses specific wavelengths of light that are non-ionizing and safe for the delicate skin of the vulva.
-
Absolutely. In fact, they are often more effective when used together. PBM can help "quiet" the overactive nerves and reduce pain, which makes it easier for your Physical Therapist to perform manual releases on the pelvic floor muscles without triggering a flare-up.
-
PBM is a powerful tool for inducing "remission" by resetting the inflammatory cycle and calming nerve overgrowth. However, because PVD often involves muscle memory and stress components, maintaining results usually requires a holistic approach, including proper vulvar skin care and stress management.
-
No. Most women feel nothing at all during a PBM session, though some report a very slight, gentle warming sensation due to increased blood flow to the area. There is no downtime, and you can return to your normal activities immediately after a session.
Provoked Vestibulodynia is a complex, physical condition, but it is not a life sentence. By addressing the root causes, inflammation, nerve sensitization, and muscle guarding we can shift the body out of a "pain loop." Photobiomodulation (PBM) offers a non-invasive, gentle path toward healing that works with your body’s natural cellular biology. If you’ve been told your pain is "normal," please know that it isn't - and there are targeted, evidence-based treatments available to help you get back to feeling like yourself.
Tracy
Hi - I’m Tracy. As a Midwife with an M.Sc (Hons), I’ve spent my career listening to women who feel dismissed by the healthcare system. My mission is to provide evidence-based tools like Red Light Therapy that help you reclaim your body and your comfort. When I’m not in the clinic or writing, I’m researching the next frontier of women’s intimate wellness to ensure no woman has to "just live" with pain.
Important Note: The information provided in this blog is for educational and informational purposes only and is not intended as medical advice, diagnosis, or treatment. While Photobiomodulation (Red Light Therapy) is supported by clinical research, individual results may vary. Always seek the advice of your Midwife, PT, Physician, or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
1. https://pubmed.ncbi.nlm.nih.gov/28970071/
2. https://academic.oup.com/jsm/article/22/4/579/8010870
3. https://www.nva.org/wp-content/uploads/2015/01/lev-sagie-LLLT.pdf
4. https://pubmed.ncbi.nlm.nih.gov/39940084/