The Science of Red Light Therapy for Wound Healing and Scar Care
Content warning: This article contains graphic clinical photos of wounds and surgical sites for educational purposes. Please proceed only if you are comfortable viewing medical images of wounds.
Red light therapy (RLT) occupies a unique space in modern medicine: it feels cutting-edge, yet it aligns perfectly with the body’s innate biological rhythms. Rather than overriding your system, the right wavelength and dose of light energize your cells to repair themselves more efficiently. While it doesn't replace standard medical care, RLT is a powerful ally that helps wounds close faster, reduces discomfort, and promotes healthier tissue regeneration for a faster recovery. I use PBM with many of my postpartum clients for perineal and cesarean wound care but what you’re about to see below (keep scrolling down) is quite mind blowing and yet not part of wound care in most countries - despite compelling evidence.
The Mechanism: How Light Supports Biological Repair
While the word laser often makes peoplel think of James Bond style lasers that cut or burn tissues, laser Photobiomodulation (PBM) is the functional opposite. Using low-energy red and near-infrared light (600 - 1,000 nm), PBM gently triggers a cellular reboot rather than using thermal force.
Inside the cell, the transformation is profound:
Enhanced Cellular Energy: Mitochondria absorb specific light wavelengths to produce ATP, the universal fuel cells require for regeneration.
Optimized Circulation: By improving microcirculation, RLT ensures oxygen and vital nutrients reach the wound site, breaking the cycle of chronic, low-grade inflammation.
Balanced Inflammation: RLT modulates inflammatory mediators, creating an ideal environment for clearing damaged debris and synthesizing new collagen.
In short: Red and near-infrared light help stressed or injured cells regain the vitality of healthy tissue.
The Evidence: What the Research Confirms
To advocate for photobiomodulation professionally, we have to look at the clinical data. It’s impressive. When used as an adjunct to standard wound care, the results are significant.
Post-Surgical Success: A 2026 systematic review of 56 randomized trials (n ≈ 4,920) found that adding near-infrared light (630–1,100 nm) to standard postoperative care significantly improved healing and lowered pain scores.
Chronic Wound Breakthroughs: 2024 meta-analyses indicate that adjunct red/infrared light can nearly double healing rates for chronic ulcers and skin wounds compared to standard dressings alone.
Structural Integrity: Controlled studies consistently show superior wound contraction and epithelialization (the formation of new skin) in RLT-treated groups.
Depth Matters: Superficial vs. Deep Tissue
A common misconception is that all red light is created equal. In reality, light penetration is dictated by physics.
Superficial Wounds (630–660 nm): Ideal for the epidermis and dermis. This includes C-section scars, perineal tears, and laparoscopic incisions. Red light at this depth excels at surface repair and collagen synthesis.
Deep Tissue (800–900 nm): Near-infrared (NIR) light penetrates deeper into muscle, fascia, and even joint capsules. This is essential for addressing deep-seated inflammation and stubborn pain.
The Solasta Advantage: Clinical Power at Home
For most superficial to moderately deep wounds, the Solasta handheld laser offers a professional-grade solution in a portable format.
Dual-Wavelength Precision: By delivering both 650 nm (Red) and 808 nm (NIR), Solasta mirrors the exact ranges used in successful clinical trials.
Coherent Laser Diodes: Unlike low-power LEDs, Solasta uses laser diodes to provide the focused, "coherent" light necessary to reach the upper muscle layers and dermal tissue.
Applications: It is the gold standard for fresh surgical scars and localized soft-tissue inflammation.
When to Seek a Clinical Specialist
While home devices are highly effective for many, very complex or "non-healing" wounds require a specialist’s oversight not a DIY approachoversight,. Chronic diabetic ulcers, radiation-damaged tissue, or deep-seated systemic issues often require:
Customized Dosimetry: Calculating specific Joules based on wound morphology.
Multi-Modal Arrays: Using high-powered, super-pulsed lasers to reach deep fascia (similar to my clinic set up).
Integrated Care: Combining light with debridement, compression, and nutritional optimization.
Blue Light and Wound Healing
You might also hear about blue‑light therapy for wounds. Blue light (around 400 - 470 nm) works very differently from red and near‑infrared light. While red/NIR light primarily supports your own cells’ energy and repair processes, blue light is being studied mainly for its antimicrobial superpowers helping reduce bacteria and biofilms on the wound surface, including some antibiotic‑resistant strains. Early research and pilot studies suggest that carefully dosed blue light can help control infection and may support healing in certain hard‑to‑heal or infected wounds, especially when used in low‑irradiance, longer “light‑bathing” protocols. At the same time, higher‑dose blue light has been shown to stress skin cells and potentially contribute to skin damage if overused, so it is not something to experiment with aggressively at home. For this blog the focus is on red and near‑infrared light for supporting the body’s healing response. If infection or chronic, non‑healing wounds are part of your story, that is a situation where working with a wound‑care or photobiomodulation specialist - who can safely combine red/NIR with carefully controlled blue‑light protocols if appropriate - is the better path.
FAQ: Red Light Therapy for Wounds
1. How soon after surgery can I start using red light therapy?
Most clinicians recommend waiting until the wound is no longer bleeding and has been cleared by your surgeon - typically within a few hours post-op. For incisions with staples or sutures, red light can be used immediately to support the surrounding tissue, provided the device does not make direct contact with an open, unshielded wound.
2. Can red light therapy help with old surgical scars?
Yes. While RLT is most effective on fresh or remodeling tissue, it can still support older scars by stimulating collagen remodeling and improving local microcirculation. This can help soften the texture of the scar, reduce redness, and improve the flexibility of the underlying fascia.
3. What is the difference between Red (650 nm) and Near-Infrared (808 nm) light?
The primary difference is depth of penetration.
Red Light (650 nm) is absorbed by the superficial layers of the skin, making it ideal for surface-level healing and skin texture.
Near-Infrared (808 nm) travels deeper into the body, reaching muscles, tendons, and even bone. Using both simultaneously, as the Solasta laser does, ensures the wound is treated from the surface down to the structural base.
4. Is it possible to "overdose" a wound with light therapy?
In the world of photobiomodulation, this is known as the Biphasic Dose Response. Essentially, there is a "sweet spot" for healing. While a low-to-moderate dose stimulates repair, an excessive dose can actually slow down the process by over-stressing the cells. Following a guided protocol is the best way to ensure optimal results.
5. Does the light need to touch the skin to work?
For a laser device like the Solasta, "contact" or "near-contact" (within 1 cm) is generally preferred. This minimizes reflection and scattering, ensuring the maximum number of photons actually reach the target tissue. However, if a wound is too sensitive for contact, the laser is powerful enough to be held slightly above the surface while still delivering a therapeutic dose.
6. Can I use red light therapy on an infected wound?
Red light therapy should be used with caution on active infections. While some studies suggest certain wavelengths have antibacterial properties, it is vital to consult your healthcare provider first. RLT is most effective as a proactive tool to prevent stalls in healing and to support the immune response in a clean wound environment.
Images of Wound Healing Progression using Laser
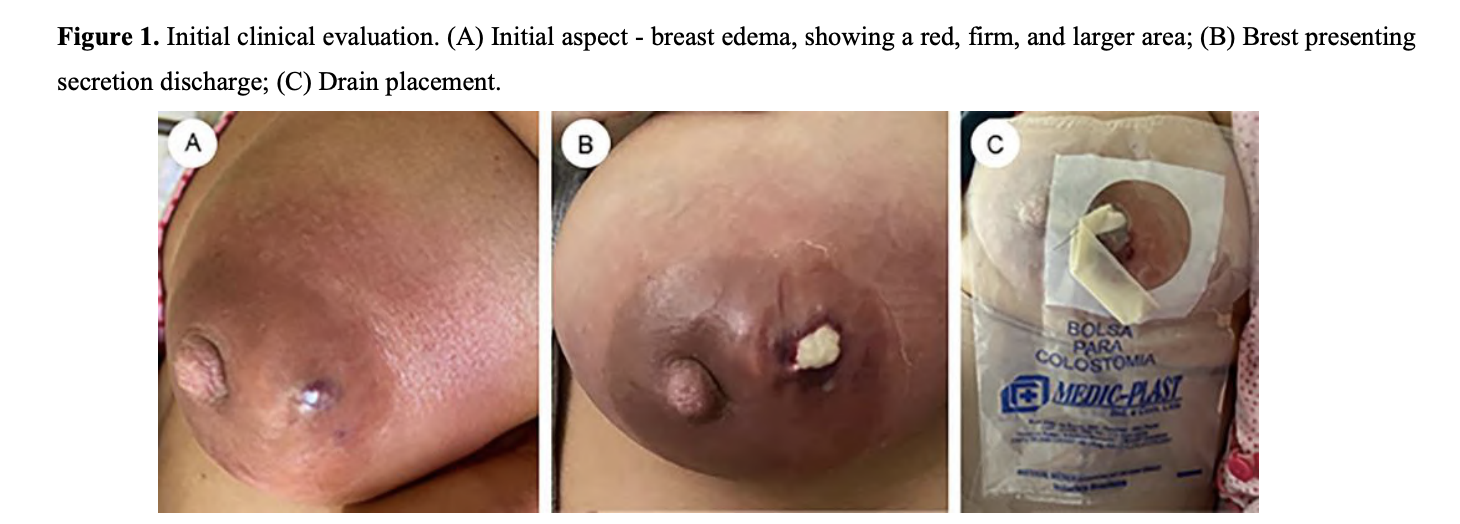
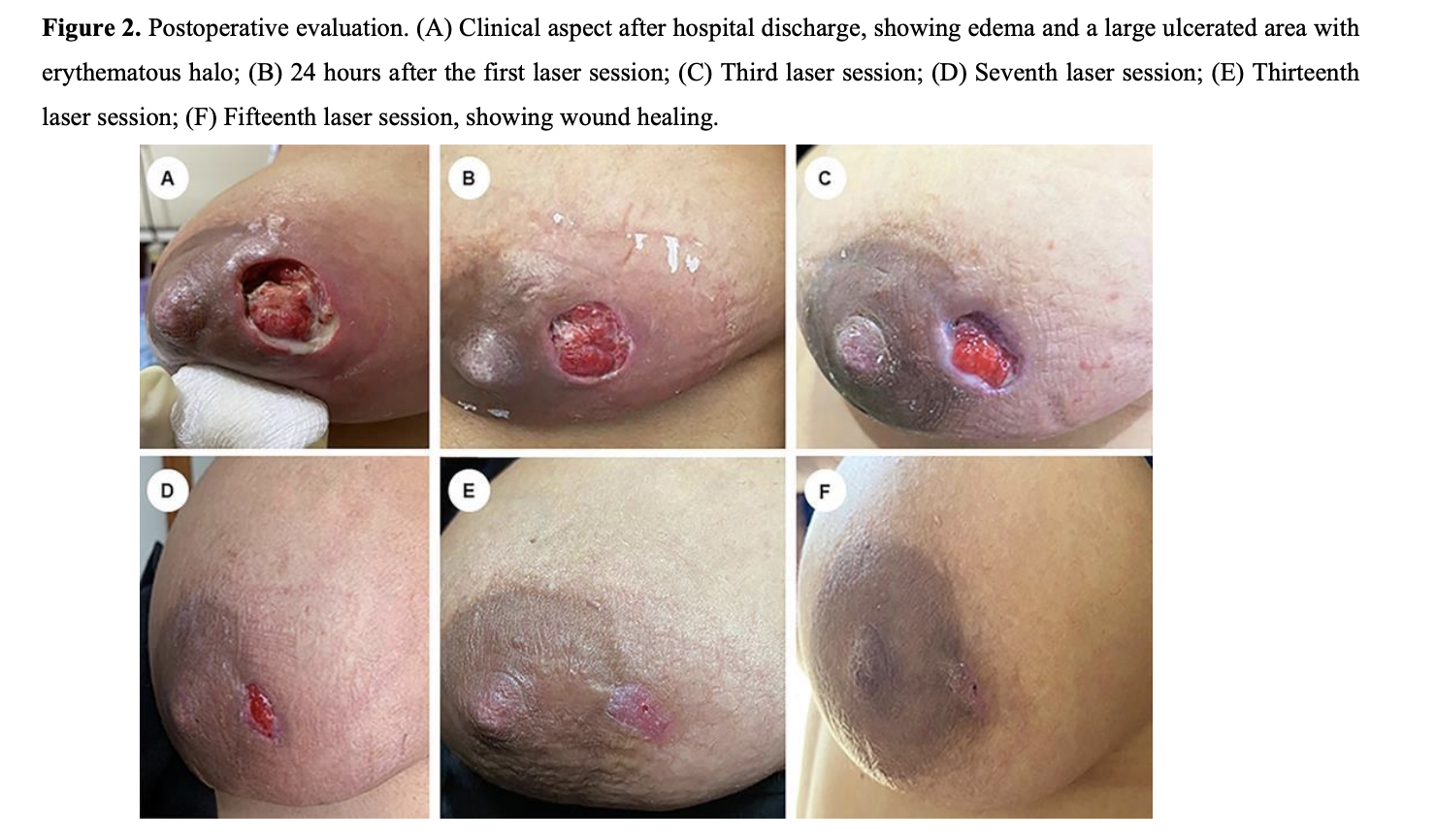
Red light laser therapy for breast abscess.
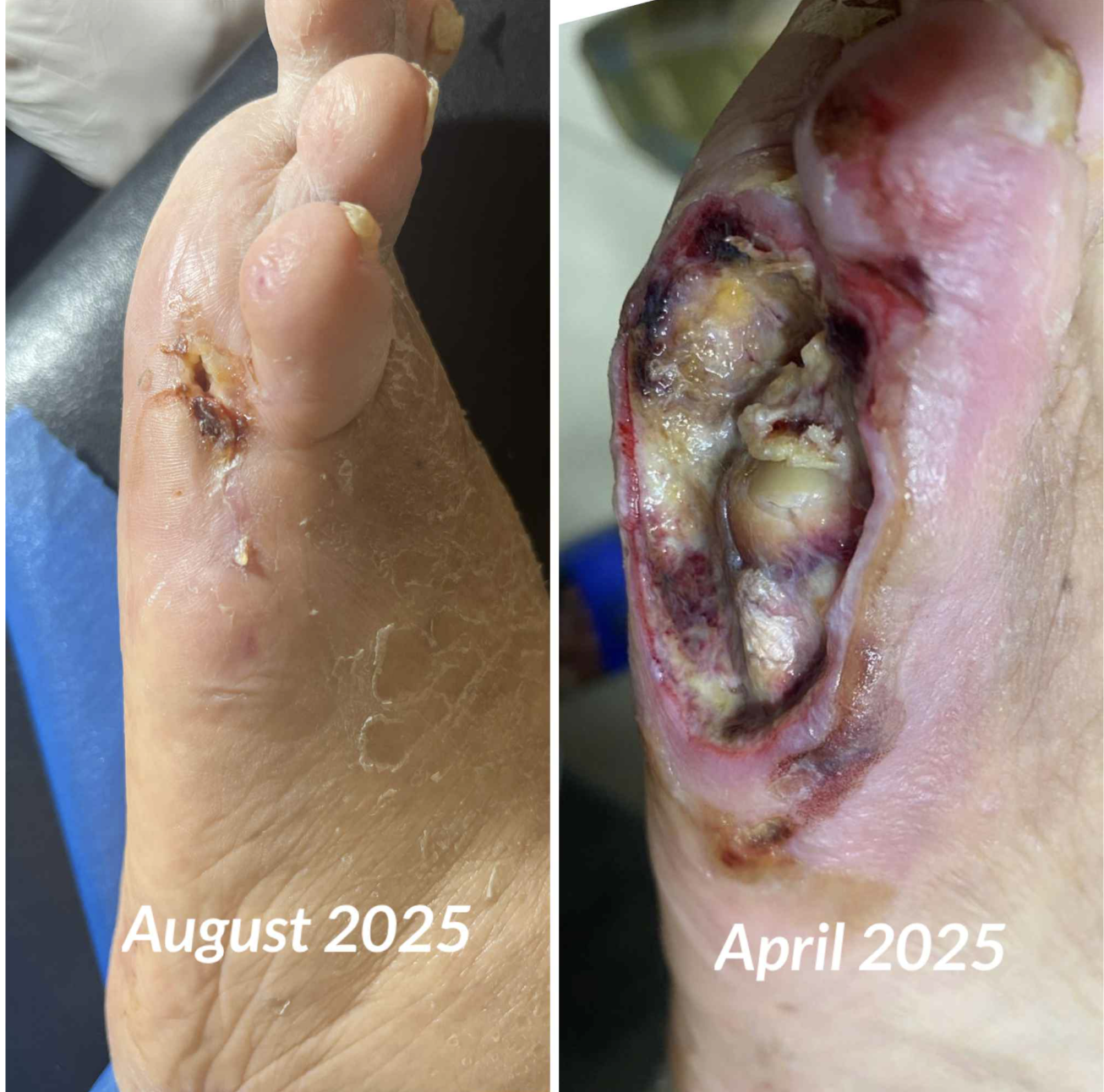
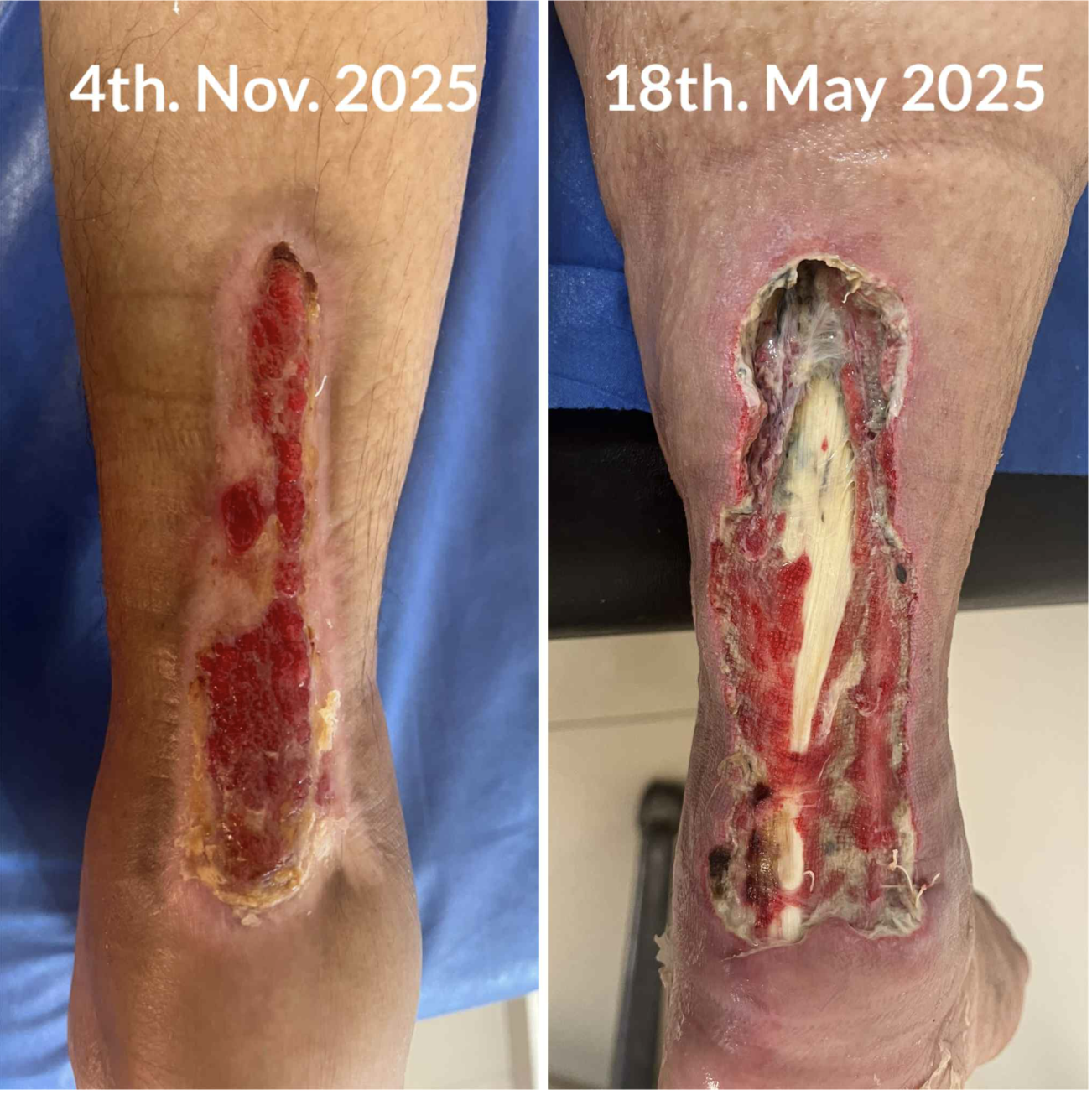
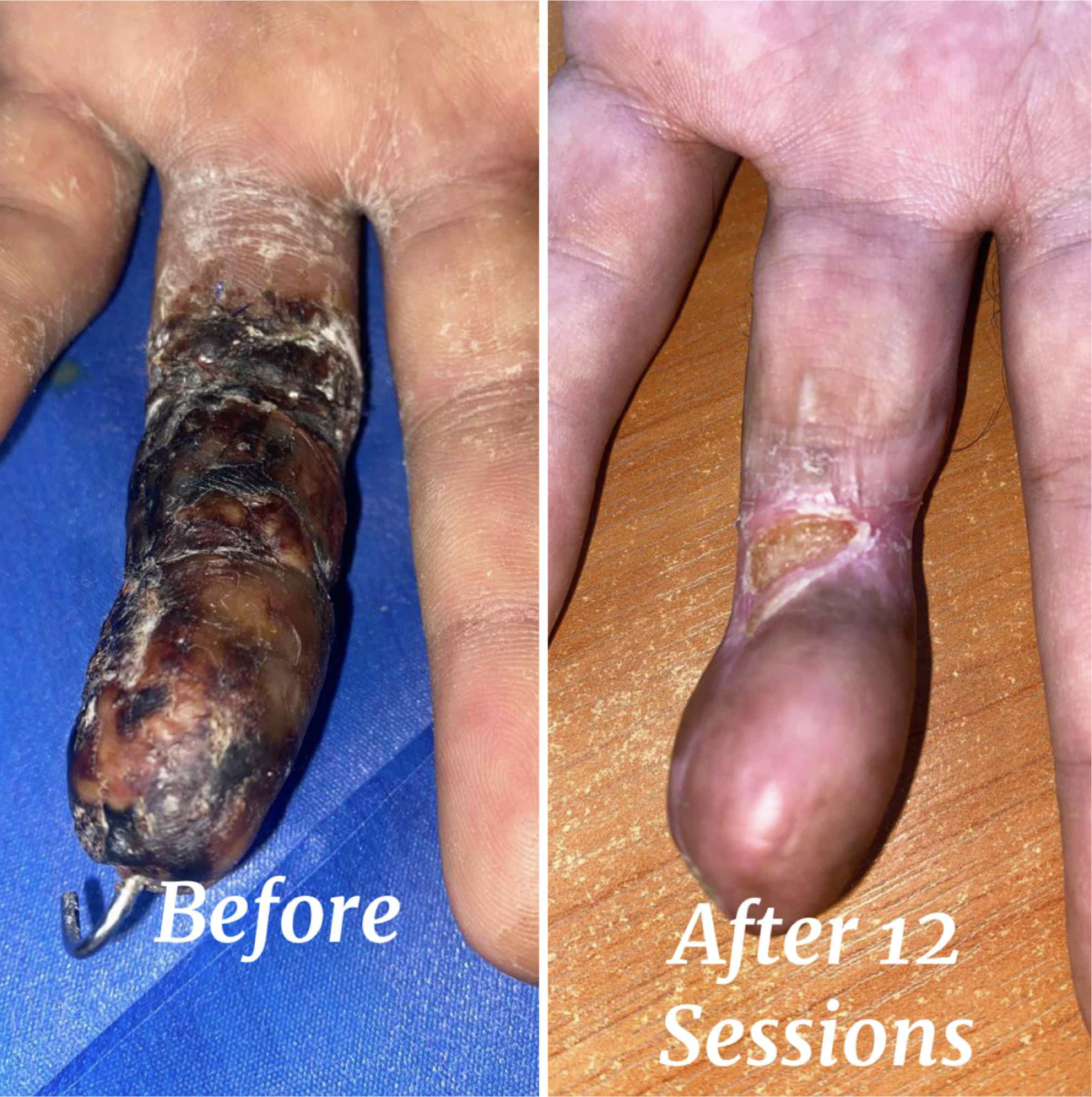
The following images are from a colleague using a Class IV clinic laser (and ozone therapy) in Egypt.
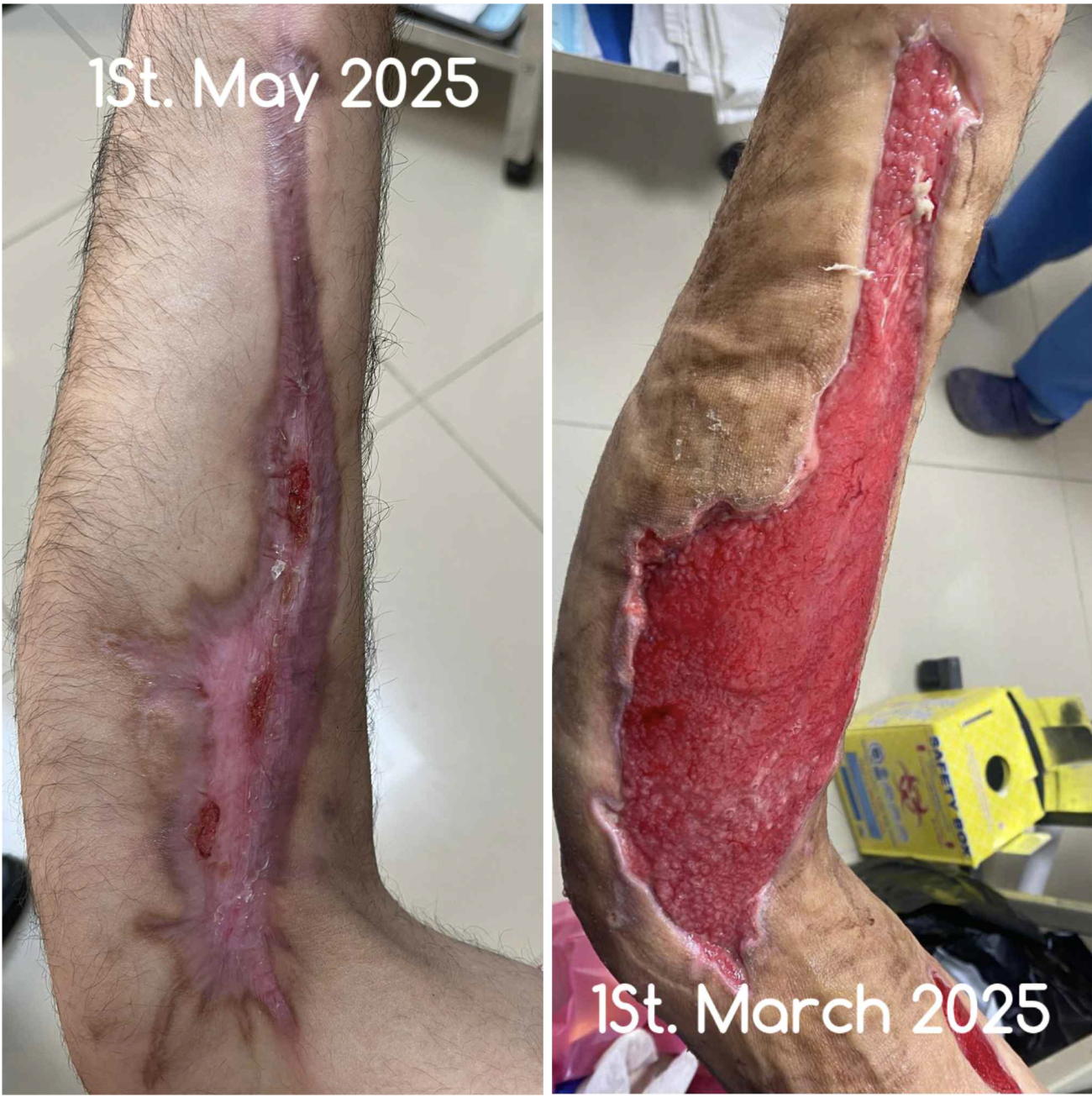
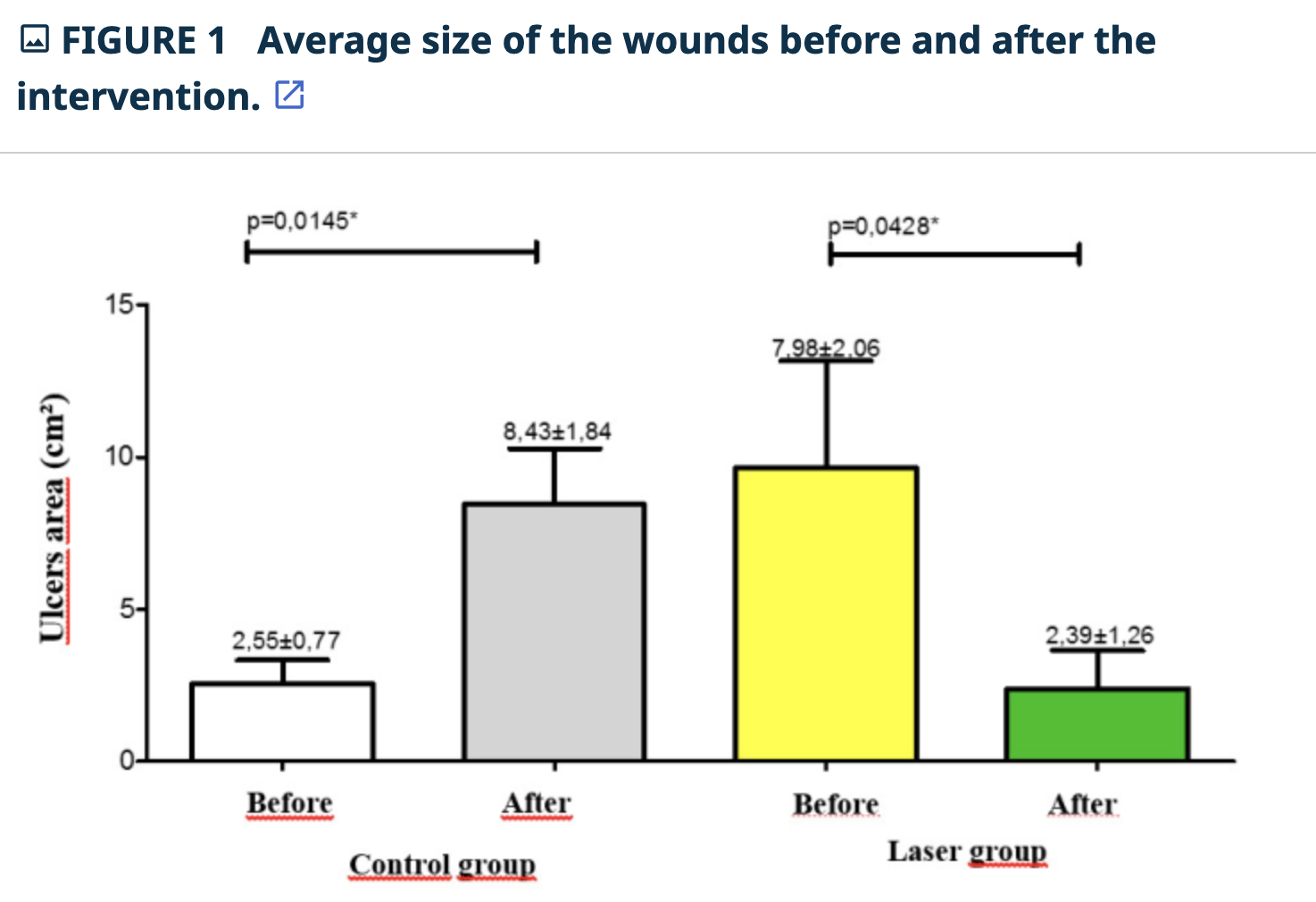
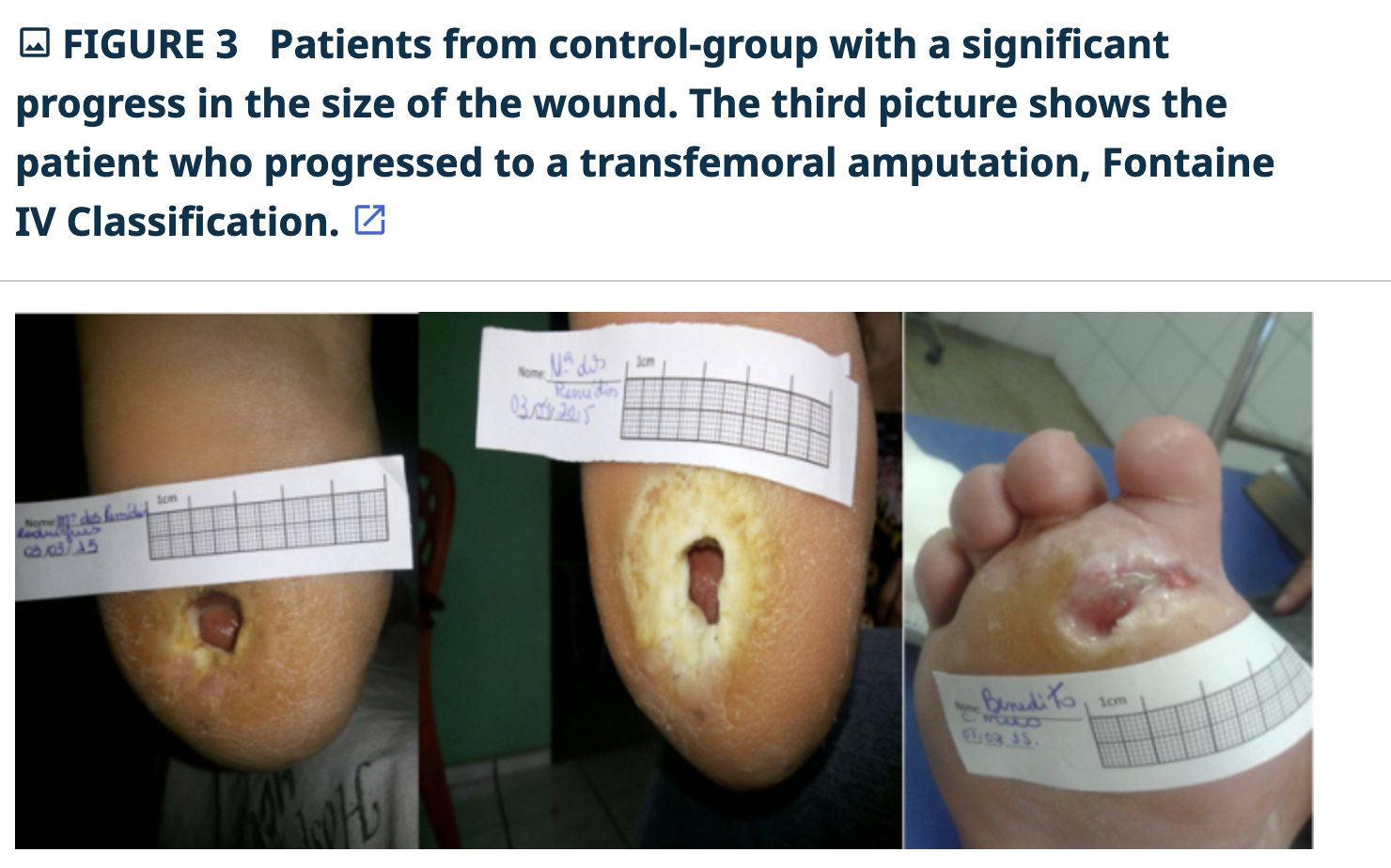
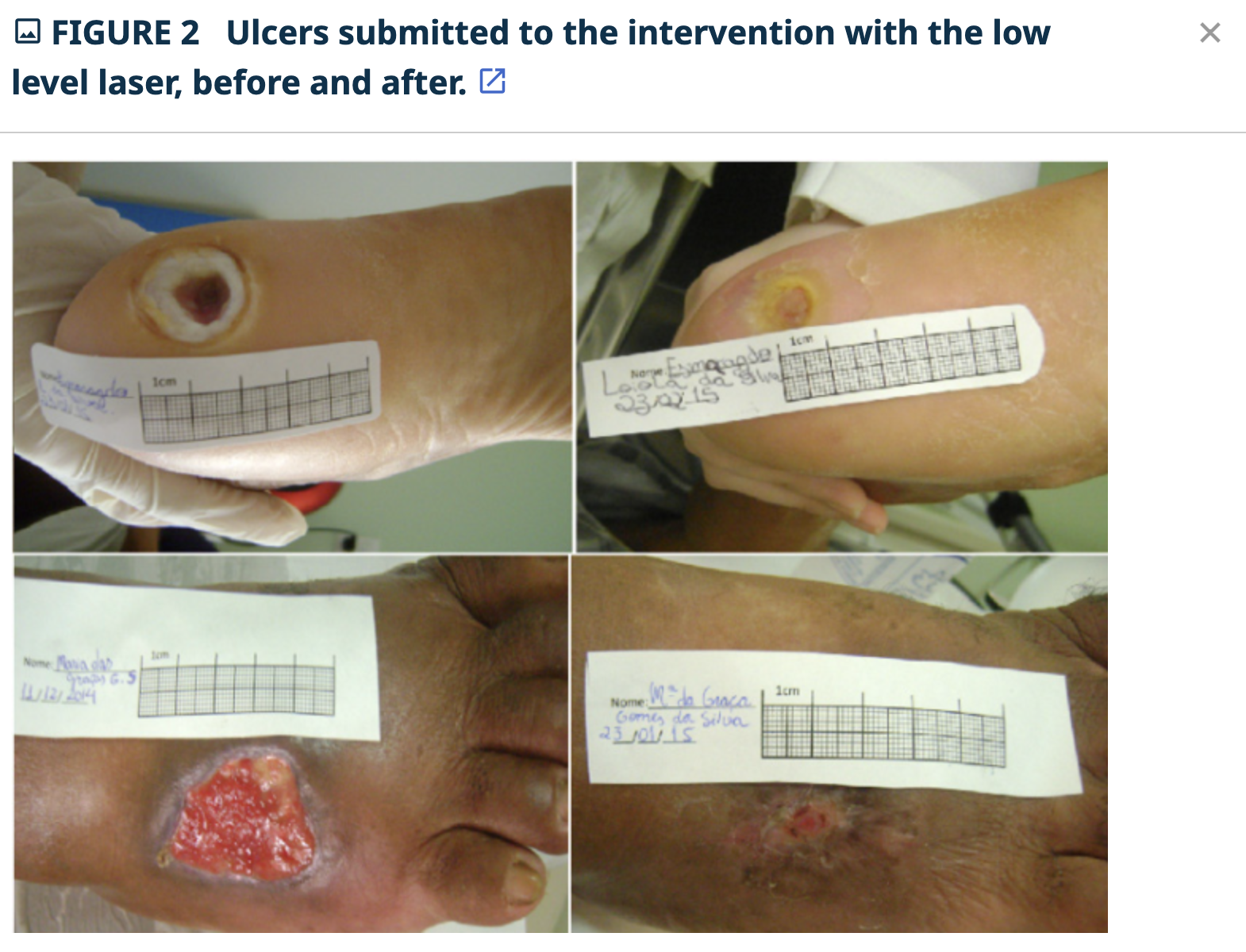
The following images are from a Brazilian study using low level laser on chronic slow healing wounds.
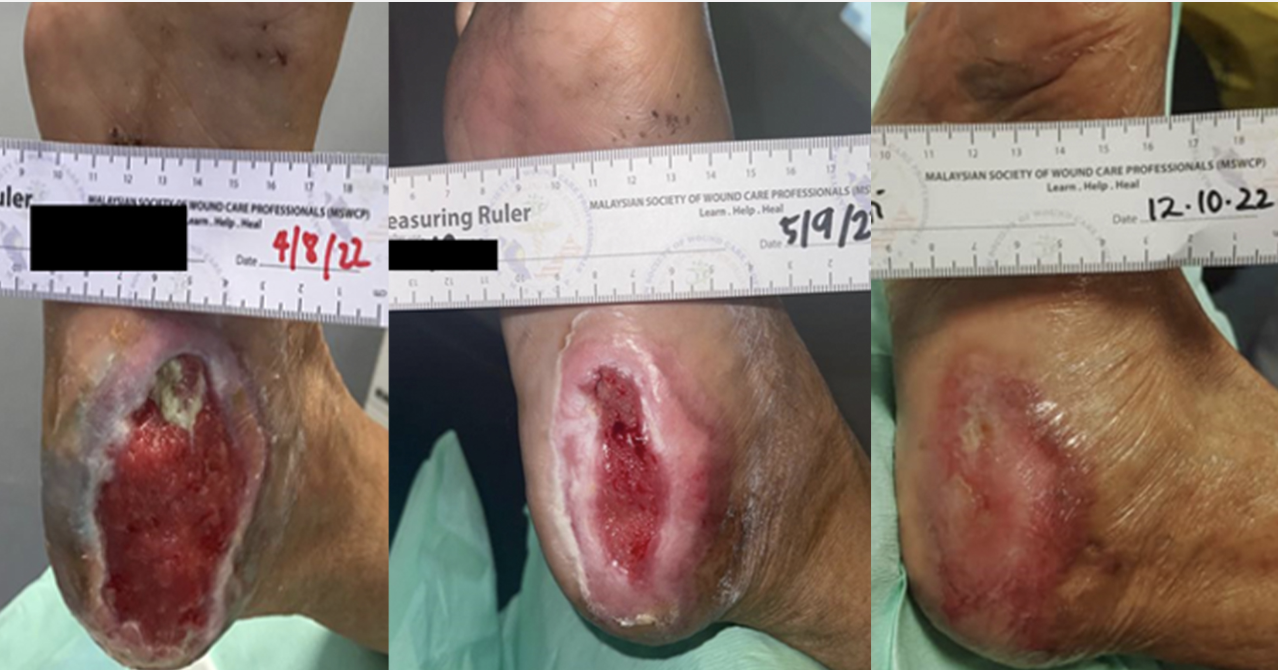
Below are images from the BLESS trial in Asia.
Chronic wound progression using photobiomodulation in a clinical setting.
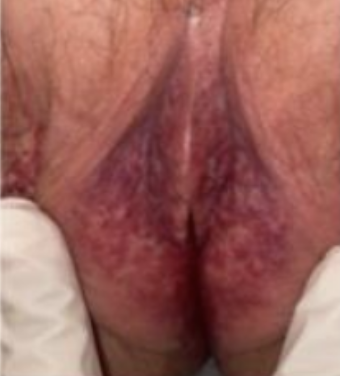
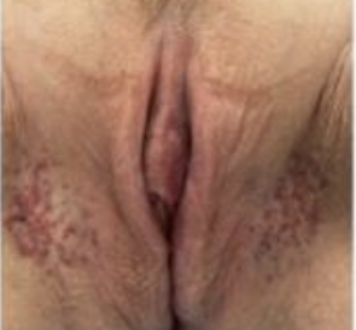
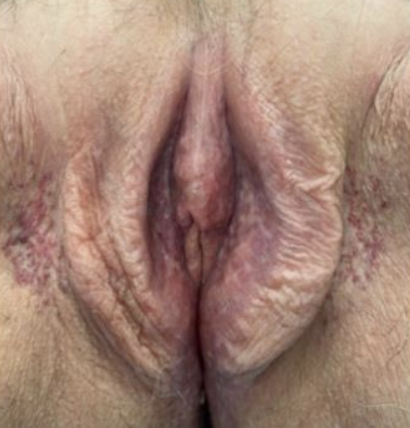
French studies using PBM for women’s intimate health
This patient was 58 and had cancer treatment for breast and anal cancer and experienced a significant improvement.
Red and near‑infrared light are not a replacement for good medical care, but they are a powerful way to partner with your body’s own healing systems. When you match the right wavelength, dose, and device to the type of wound you are dealing with, you can often ease pain, support healthier tissue repair, and feel more in control of your recovery journey.
For most everyday and postpartum wounds, a clinical‑grade home device like the Solasta laser gives you accessible, evidence‑aligned support right where you need it. When wounds are chronic, deep, or simply not behaving the way they should, that is your cue to bring in a specialist who can combine red/NIR (and sometimes carefully dosed blue light) with comprehensive wound care for truly deeper change.
Wherever you are on that spectrum, the message is the same: you do not have to “wait and see” and hope for the best. With the right guidance and the right light, you can take an active, informed role in how your body heals.
Tracy
Red light therapy for wound healing and photobiomodulation for scars, Solasta home laser vs. professional laser clinics using infrared light for surgical recovery.